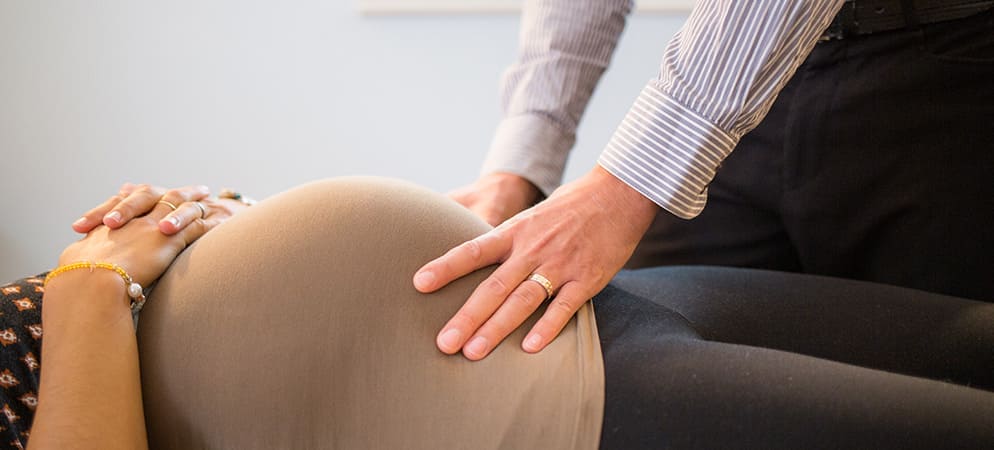
You can therefore call on these courteous, warm and competent professionals in order to receive treatments adapted to all the members of your family, whether you consult for a strain, tendonitis, carpal tunnel syndrome, muscle weakness, sciatic nerve pain, recurrent headaches, herniated disc, joint pain (wrist, shoulder, hip, knees, ankle, etc.) and more.

Chiropractor in Ste-Rose, Laval
Don't let pain affect your daily activities!
Does pain affect you on a daily basis and prevent you from carrying out your activities? Is your athletic performance affected by physical discomfort? Does your toddler seem uncomfortable or restricted in his development?
In all these cases and much more, chiropractic can help you! This natural approach aims to relieve tension without resorting to medication or surgery. Our experts in postural problems and musculoskeletal or neurological disorders, doctors of chiropractic Étienne Lefebvre, Sandra Aresteanu and Marc Fortier, offer therapeutic care aimed at the prevention, diagnosis and treatment of your pain or lack of mobility, and this, no matter your age category or lifestyle!
As soon as muscle, joint or other pain persists, call on the chiropractors at the Chiro-Santé clinic in Ste-Rose, your experts in overall health and pain management!
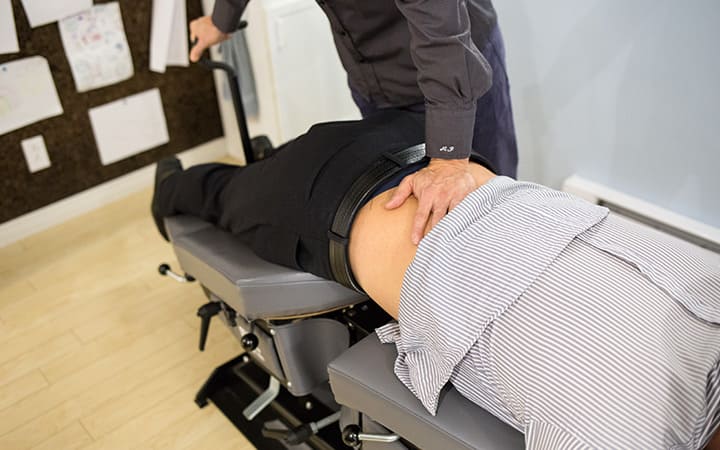


Why should I choose the services of the Chiro-Santé clinic in Laval?
Renowned chiropractors
Dr Étienne Lefebvre, Dre Sandra Aresteanu and Dr Marc Fortier all hold a doctorate degree in chiropractic, in addition to being members of the Ordre des chiropraticiens du Québec. Even more, they have perfected their knowledge and refined their techniques during their 15 to 25 years of practice!
Personalized treatments
Basing their interventions on effective and non-medicinal therapeutic methods, our chiropractors adopt a personalized approach based on your goals. They will listen to your needs in order to offer you services adapted to your age, your condition and your level of tolerance.
A relationship based on trust
Trust is the basis of the relationship that your Chiro-Santé clinic therapist wishes to build with you. In doing so, he will be able to understand your health problem as a whole and offer you a tailor-made program so that your experience with the clinic is pleasant and, above all, successful!
A service accessible to all
Although our chiropractors have certain specialties, the services of our chiropractic clinic in Laval are intended for all types of clienteles, from newborns to the elderly, including pregnant women, injured workers or athletes! All of our patients will receive the highest quality service.
We improve the well-being of residents of Ste-Rose, Fabreville, Auteuil, Vimont and everywhere in Laval!
Whether you suffer from muscle, joint, skeletal or neurological pain, we offer treatments and advice aimed at reducing your suffering while promoting healthy lifestyles!
Our chiropractors

Dr Étienne Lefebvre,
doctor of chiropractic
specialized with athletes
Passionate about sports since a young age, he honed his knowledge in sports chiropractic through additional training in applied kinesiology, allowing him to provide specialized services to athletes of all ages suffering from issues like muscle strains or sprains, among others.

Dre Sandra Aresteanu,
doctor of chiropractic
specialized with pregnant women, newborns and children
Focused on children and pregnant women, her practice is firmly supported by her additional training in pediatric and obstetric care provided by the International Chiropractic Pediatric Association, as well as her many years of work at the ABChiropratique clinic in Vaudreuil and the Chiro-Santé clinic in Sainte-Rose.

Dr Marc Fortier,
doctor of chiropractic
Having practiced in various clinics across Western Canada and the Magdalen Islands, he has accumulated a wealth of experience that has allowed him to refine his manual therapy techniques to better assist his patients. He has also served as a neuroanatomy professor at a massage therapy school in the Ottawa region.
Our techniques

At the Chiro-Santé clinic of Laval, we make it a point to adapt our practice to the client who uses our services. Thus, our therapeutic approach will not be the same for a newborn with a motor development delay as for an elderly person suffering from osteoporosis or arthritis. This is why we master a wide range of techniques and treatment methods. Here is an overview.
Complementary care at your service

We are pleased to welcome Frédéric Maréchal, a kinesiologist, to our team. His complementary approach and expertise allow us to offer you treatments and interventions in kinesiology, therapeutic massage, and physical therapy at our clinic in Ste-Rose, Laval.
Territory covered by the Chiro-Santé clinic in Laval
Although located in the Ste-Rose district, the Chiro-Santé clinic offers its services to residents and workers from all neighborhoods of Laval :


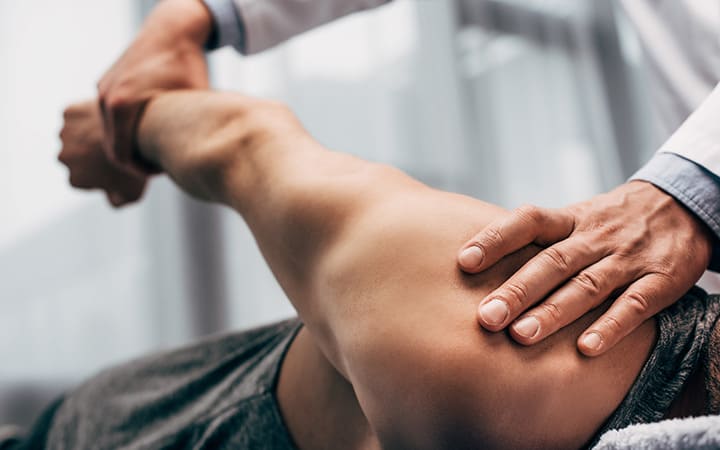
Take another step towards a return to balance : contact us!
Does your pain and lack of mobility affect your well-being? If you live or work in Ste-Rose, Fabreville, Auteuil, Vimont and elsewhere in Laval, our professionals are there for you.